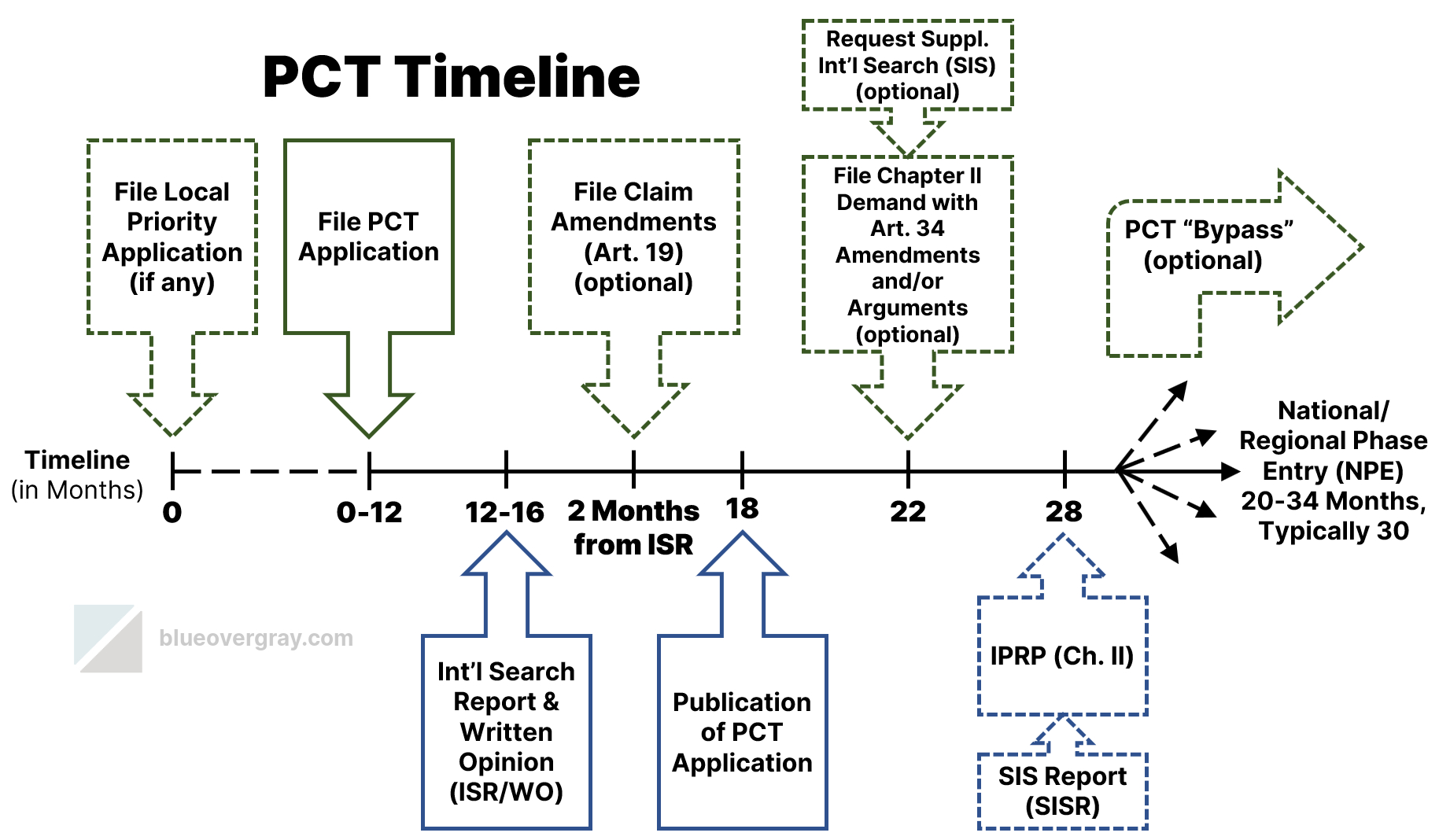
Since the No Surprises Act became effective on January 1, 2022, several disputes have arisen that challenge the weight given to the Qualifying Payment Amount (QPA) in the Independent Dispute Resolution (IDR) process. 
We will share additional details as we acquire more information and develop an action plan for addressing the end of the Emergencies within the next few weeks.ĭepartments Suspend Surprise Medical Billing Independent Dispute Resolution (IDR) Payment Determinations WebTPA will follow all updates and the effects on the plan’s processes administered by WebTPA and your plan members. It is also unknown if an HDHP can maintain its qualified plan status with the IRS, while providing telehealth services without cost sharing prior to meeting the plan deductible, after July 10, 2023, or if this be allowed to continue for the remainder of the plan year.Īdditional public and industry communications are anticipated. It is uncertain to what extent telehealth benefits may be affected by the end of the Emergencies. Under the category of preventive care, vaccines for the coronavirus will continue to be covered at 100% without member cost share. Prescribed and over the counter COVID-19 tests are covered under the PHE rules, but the end of the emergency may signal that over-the-counter tests will no longer be covered under group health plans and insurance policies and prescribed tests may include a member cost share amount. The time frame to request an external review or provide information that would perfect an external review.The claims and appeal submission timeframes as provided by plans.The 60-day notification period for a COBRA beneficiary to notify a plan of a qualifying event or determination of disability.The 30-day period to pay COBRA premiums. 
The 60-day election period for COBRA initial enrollment.The 14-day period to offer coverage to newly eligible COBRA beneficiaries.The 30-day or 60-day HIPAA Special Enrollment period, such as the addition of a new spouse or newborn child.Currently, tolling periods are the lesser of an additional one year after the event’s deadline or 60 days from the end of the National Health Emergency, which we now know is July 10, 2023. Under the National Health Emergency rules, deadlines for specific events are extended and a separate tolling period for each event is applied and these extensions will soon cease. Group health plans and issuers are studying what this means for medical plan related coverages and processes. The Biden Administration is extending the expiration date to May 11, 2023, to align with its commitment to give a minimum of 60 days' notice prior to the end of the emergencies. Reach out insurance for appeal status.The COVID-19 National Health Emergency and Public Health Emergency (PHE) were to expire on March 1 and April 11, 2023, respectively. If previous notes states, appeal is already sent.If we have clearing house acknowledgement date, we can try and reprocess the claim over a call.If claim history states the claim was submitted to wrong insurance or submitted to the correct insurance but not received, appeal the claim with screen shots of submission as proof of timely filing(POTF) and copy of clearing house acknowledgement report can also be used.If the first submission was after the filing limit, adjust the balance as per client instructions. Review the application to find out the date of first submission.Whenever claim denied as CO 29-The time limit for filing has expired, then follow the below steps: If claims submitted after the timely frame set by insurances, then those claims will be denied by insurance companies as CO 29-The time limit for filing has expired. Timely Filing Limit is the time frame set by insurance companies and provider has to submit health care claims to respective insurance company within the set time frame for reimbursement of the claims.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
